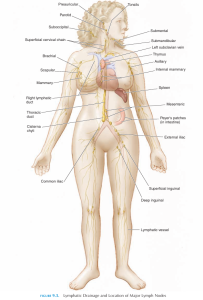
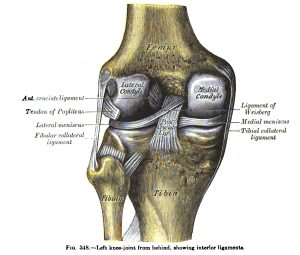
What is the Lymph system?
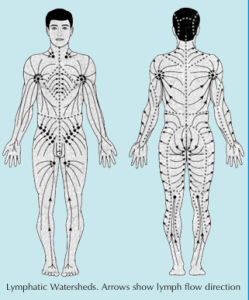
Lymph system is essentially a complex network of channels, which drain fluids and proteins from the interstitial spaces of the body’s organs and tissues and transport them to the lymph nodes. Lymph from most parts of the body finally drains into the venous circulation via the thoracic duct. Numerous valves are present along the lymphatic collecting vessels and trunks, and they aid in directing lymphatic drainage from the periphery toward the subclavian vein. There are approximately 30–35 valves only in the thoracic duct.
The lymph consist proteins, lipids and enzymes.
Most of the protein in lymph is derived from plasma proteins by filtration, diffusion, and vesicular transport.
The lipids in lymph and plasma consist of triglycerides, phospholipids, cholesterolesters, fatty acids, and free cholesterol. Lipid concentrations change markedly after meals. The lipid content of intestinal and liver lymph is much higher than in other lymph.
Enzymes normally present in plasma are also present in lymph, but generally at lower concentrations than in plasma.
The great majority of cells in human peripheral lymph are lymphocytes.
The lymph is responsible for defence against infection and disease, and to help remove excess water from the tissue spaces.
Lymph vessels have one-way valves to help direct the fluid. Lymph is also propelled to a large extent by the passive and active movements of skeletal muscles. In addition, the pulsation of arteries lying close to the lymph vessels helps propel the lymph. Another important mechanism that draws the lymph upward is the respiratory movements. When a person inspires, the pressure drops in the thorax and increases in the abdomen. This difference in pressure is sufficient to “suck” the lymph into the thorax and the venous system.
Changes in posture, passive compression, and massage can also aid lymph flow. The smooth wall muscles of the lymphatic vessels also help move lymph by contracting when distended. The rate of flow increases with physical activity. It has been estimated that about 2–4 liters of lymphatic fluid and the equivalent of 25% to 50% of the total circulating plasma protein is returned to the circulation every day.
What is lymphedema?
Lymphedema may be classified as primary (idiopathic) or secondary, depending on its etiology. Primary edema may be congenital or a result of unknown causes. Secondary lymphedema may be a result of obstruction or trauma to the lymphatic system (e.g., surgical removal of lymph nodes, radiotherapy, or infection).
Lymphostasis, or stagnation of lymph, results when normal lymph flow is impeded. It may be caused by congenital malformation of the lymph vessels; mechanical obstruction, such as extrinsic or intrinsic compression; traumatic or surgical injuries; radiation; or inflammation of lymphatic vessels and nodes. Removal of lymph nodes and radiotherapy in the treatment of cancer, infection (e.g., filariasis), and trauma are common causes of lymphostasis.
Lymphedema is the accumulation of lymph that results from lymphostasis. Protein and fluid tend to accumulate in the interstitial fluid compartment (lymphedema). With time, the protein precipitates, triggering proliferation of fibroblasts and formation and accumulation of elastic and collagen fibers with resultant thickening of connective tissue and hardening and enlargement of the structure. Lymph vessels caught in the fibrous tissue perpetuate the situation. When the lymphatic vessels dilate, the valves become incompetent and lymph flows backward. The pressure in the lymphatic capillaries pushes lymph from the vessels into the interstitial compartment and, at times, into the blood capillaries.
Lymph also flows through collateral anastomotic channels that exist between various groups of collecting ducts. They may also drain backward through collaterals that exist between lymphatic trunks of other regions. For example, if the axillary nodes are removed, lymph may drain backward through collaterals to the deltoid group of collecting ducts that drain directly into the supraclavicular lymph nodes. Regeneration of lymph vessels can also occur to compensate for lymphostasis. For example, when a lymph node is excised, a dense network of capillary vessels is formed to connect the afferent and efferent vessels.
Signs and Symptoms of Edema
 Swelling
Swelling- Pain
- Heaviness
- Reduced mobility
- Strain on associated joints and muscles
- Tightness of overlying skin
- Skin changes (e.g., increased susceptibility to skin breakdown, infection, and injury; delayed wound healing; lower skin temperature as a result of reduced blood flow in the area
- Sensory disturbances of the hand and foot
- Psychological disturbances owing to alterations in body image, sexuality, and social acceptance
Benefits of massage and exercises
The massage technique used for lymphedema is called manual lymph drainage.
Massage therapists can apply the massage strokes along the direction of lymph drainage and speed lymph movement. Massage has positive effects on lymph drainage. It is believed that the effects of massage are equal to the circulatory effects produced by the contraction of muscles.
Appropriate strokes and drainage techniques can help with the movement of lymph and reduce edema. Passive exercise often used in conjunction with massage also encourages lymph drainage. Massage over lymph nodes can speed lymph drainage and hasten the resolution of swelling resulting from adhesions. Massage has been shown to be particularly effective in relieving postsurgical swelling and pain and for enhancing the rate and quality of healing.
The removal of edema fluid reduces the incidence of fibrosis in the location. In addition, pain can be relieved by removing those chemicals and waste products dissolved in the fluid that stimulate pain receptors.
Pneumatic massage therapy refers to the use of pneumatic devices to reduce edema. Here, a sleeve with multiple cuffs is applied over the edematous limb and compressed air is sent into the sleeve. By systematically inflating and deflating the various cuffs, pressure is applied to the sub cutaneous tissue in a wavelike pattern, facilitating lymph drainage.
Following massage, the area is bandaged, using low-stretch bandages to increase tissue pressure, support the connective tissue, and maintain the reduction obtained from the massage. Active exercise programs specifically designed to clear proximal areas prior to distal areas further help drain lymph. At times, a pneumatic pump (mercury compression pump) may be used to assist drainage.

Contraindications to Lymph Drainage Techniques
- Other techniques, which can help the lymph system are:
- -deep breathing exercises
- -upper and lower limb exercises
- -using a brush with the direction of the lymph system on your skin
- – swimming
- – Pneumatic devices
- – kinesiotape, bandaging
Naturopathic Healing can help your lymph system. Naturopathic Healing is offering lymphatic drainage massage with combination with exercises and kinesiotape.
References:
Lymphatic Mapping and Probe Applications in Oncology
The Massage Connection ANATOMY AND PHYSIOLOGY- Kalyani Premkumar




 Swelling
Swelling